
How to choose the perfect menstrual cup for you?
16 de April de 2026
How to Remove Female Pubic Hair at Home – Complete Guide with Images
11 de May de 2026
This article is informative and does not substitute for medical advice. Consult your gynecologist if you have any questions about your health.
There is something that many of us have known since adolescence and is rarely explained well: that period pain is not just "women's issues" nor something to endure in silence. It has a name, it has a mechanism, and in most cases, it has a solution. Or at least, real relief.
If you've ever wondered why it hurts so much —or why your friend feels almost no pain— here’s an honest explanation, without dramatics or miracle promises.
Dysmenorrhea: types and causes
The medical term for menstrual pain is dysmenorrhea, and it affects between 50% and 80% of people with a uterus at some point in their lives. It’s not an exaggeration or a rarity: it’s the most common gynecological condition, yet it remains quite misunderstood.
There are two main types:
- Primary dysmenorrhea — This is the most common type. It occurs without any underlying disease and usually begins one or two days before menstruation, peaking in the first 24-48 hours. The main culprit is prostaglandins, substances that the body produces to help the uterus contract and expel the endometrium. When levels are very high, contractions are more intense, local circulation decreases, and pain spikes. Some people also experience nausea, headaches, or diarrhea due to this same mechanism.
- Secondary dysmenorrhea — Here, the pain is related to a medical condition: endometriosis, adenomyosis, uterine fibroids, ovarian cysts, or pelvic inflammatory disease, among others. It tends to be more persistent, occurring outside the usual period of cramps and not responding as well to standard pain relievers.
The intensity of the pain also varies according to factors such as age (it usually improves with age or after pregnancy), stress, sedentary lifestyle, and diet.
When pain is NOT normal
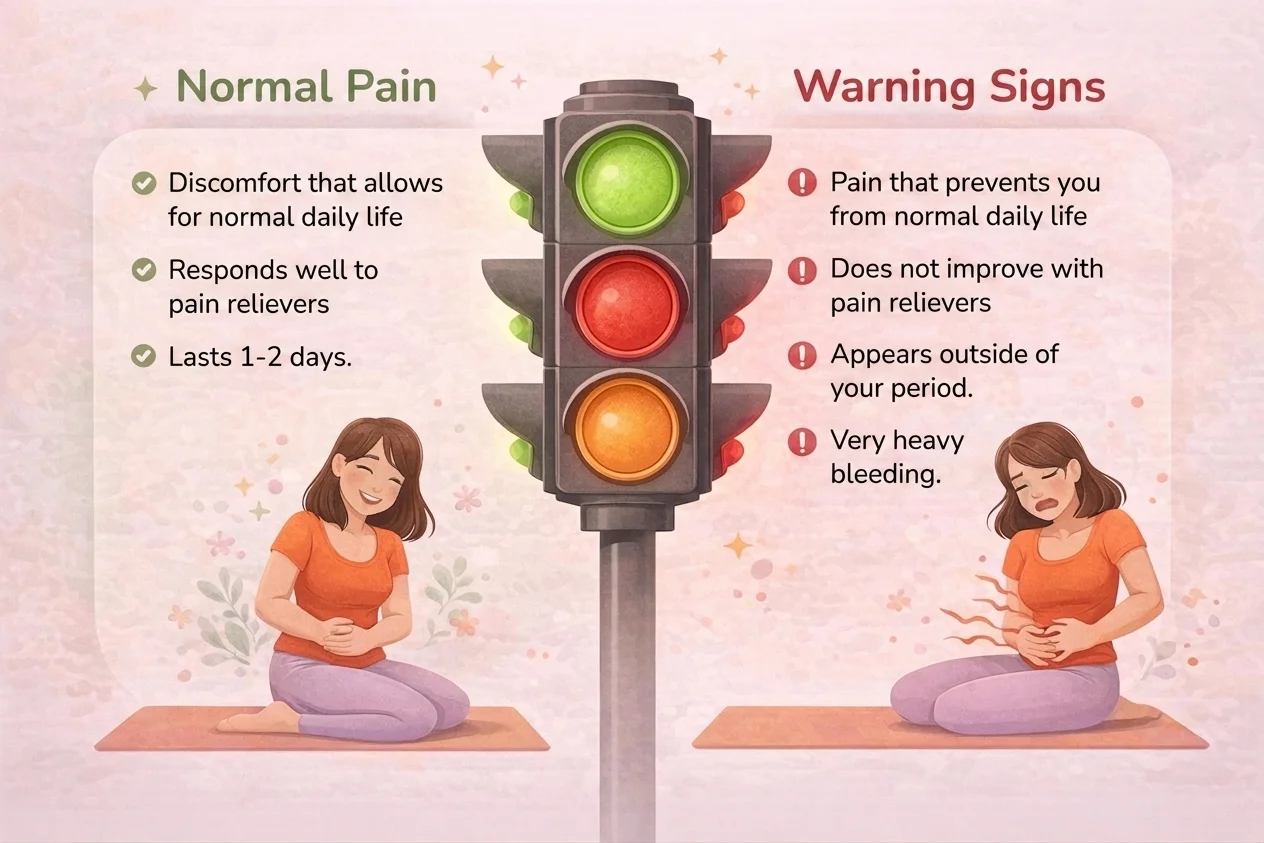
Your period can be painful. That’s real. But there are signs that deserve medical attention and should not be ignored:
- The pain is so intense that it prevents you from living normally for more than a day or two.
- Common pain relievers (ibuprofen, acetaminophen) do not work for you.
- The pain also appears outside of your menstrual period, during ovulation or when having sexual intercourse.
- You notice that the pain progressively worsens with each cycle.
- You have very heavy bleeding, large clots, or very irregular cycles.
These symptoms may indicate endometriosis or other conditions that require diagnosis. If you are not sure what a normal period is for you, that article can help you gain more context before your consultation.
Natural remedies with evidence
Not everything circulating on the internet about menstrual pain is scientifically backed. Here are the ones that are, to varying degrees:
Local heat. Applying heat to the abdomen is one of the most supported methods. Several studies have shown that a heat pack or electric heating pad can be as effective as ibuprofen for primary dysmenorrhea, and without side effects. It works because heat relaxes the uterine muscles and improves local circulation.
Ibuprofen and non-steroidal anti-inflammatory drugs. They are the first-line treatment recommended by most clinical guidelines. They work by blocking the production of prostaglandins, not just masking the pain. Taking them in advance —just when menstruation starts or a little before, if the cycle is predictable— is usually more effective than waiting for the pain to become intense. They are not bad to take occasionally; the key is not to overdo it.
Magnesium. There are studies suggesting that magnesium supplementation can reduce the intensity of menstrual pain, possibly because it helps relax smooth muscle. It’s not a miracle solution, but it can be a useful supplement, especially for those with a deficiency.
Omega-3. Omega-3 fatty acids have anti-inflammatory effects, and some clinical trials have observed that they reduce dysmenorrhea when taken continuously. They are found in fatty fish, walnuts, and flaxseeds, although supplements are also available.
Exercises that relieve cramps
I know that when you have cramps, the last thing you want to do is move. But moderate exercise —especially certain types— can make a real difference.
Movement increases the release of endorphins (natural painkillers), improves pelvic circulation, and reduces muscle tension. It doesn’t have to be intense; in fact, on days with more pain, gentle movement works better.

Yoga poses that help:
- Child's Pose (Balasana): Kneeling, sit on your heels and stretch your arms forward with your forehead resting on the ground. Hold for 1-2 minutes. Decompress the lower back and relax the abdomen.
- Cat-Cow Pose (Marjaryasana-Bitilasana): On all fours, alternate arching and sinking your back with each breath. Mobilize the pelvis and relieve tension.
- Legs Up the Wall (Viparita Karani): Lie down with your legs resting vertically against the wall. It promotes venous return and has a notably calming effect.
- Supine Twist: Lying on your back, bring your knees to your chest and then tilt them to one side while turning your head to the other. Repeat on both sides.
- Pigeon Pose (Eka Pada Rajakapotasana): More demanding, but very effective for releasing tension in the hip and psoas, which is often tight in people with frequent cramps.
Walking also works well when the pain is mild. And if you have regular cycles, doing moderate cardiovascular exercise in the weeks leading up to your period can reduce the intensity of cramps the following month.
Anti-inflammatory diet
What you eat in the days leading up to your period can influence more than it seems. It's not about a miracle diet, but about reducing foods that promote inflammation and increasing those that modulate it.
Better to reduce:
- Refined sugar and ultra-processed foods.
- Alcohol, especially in the days leading up to your period.
- Excess caffeine, which can increase vascular tension.
- Excess salt, which promotes fluid retention and worsens bloating.
Better to include:
- Leafy greens (spinach, Swiss chard, kale): rich in magnesium and vitamin K.
- Fatty fish (salmon, sardines, mackerel): a source of omega-3.
- Nuts and seeds, especially walnuts and flaxseeds.
- Ginger: has anti-inflammatory properties and can reduce nausea associated with menstruation. In tea or added to meals is an easy way to incorporate it.
- Turmeric: another natural anti-inflammatory. Combine it with black pepper to enhance absorption.
Staying well-hydrated also helps: water reduces retention and can alleviate the feeling of pelvic heaviness.
Menstrual cup and reduction of discomfort
This surprises many people, but it makes sense.
Tampons, by absorbing the flow, also absorb the natural moisture of the vaginal mucosa and create slight internal pressure. In some people, this can worsen the feeling of tension or discomfort during menstruation. Additionally, the materials of some tampons can cause irritation or reactions in sensitive skin.
Our menstrual cup works differently: it collects the flow without absorbing it, does not alter the pH or vaginal moisture, and does not create pressure on the walls. For many people, this makes a tangible difference.
In a survey we conducted with 500 users, 64% reported less discomfort using the cup compared to tampons. This is not a clinical data point, but it reflects an experience that many recognize: the change not only affects practical comfort but also how one feels during their period overall.
If you have questions about which menstrual cup to choose or if the menstrual disc might be a better option for you, in our store you have size guides and comparisons. The menstrual disc is another alternative worth exploring, especially if you have a low cervix or are looking for more capacity.
Why choose us?
At Papayacup we have been accompanying people in the process of better understanding their period —with real information, without taboos and without empty promises.
Our menstrual cups are made from high-quality medical silicone, available in two sizes to fit different bodies and life stages, and we answer questions with a level of detail that few brands offer.
But perhaps the most valuable aspect is not the product itself, but what comes with it: learning to listen to your own body. Knowing when the pain is tolerable and when to seek help. Understanding that menstruation doesn't have to be a lost week each month.
Frequently asked questions about menstrual pain
A certain degree of discomfort is common, but pain that prevents you from living normally should not be normalized. If you need high doses of painkillers regularly or the pain affects your daily life, it's worth consulting a professional.
If the pain worsens over time, does not respond to ibuprofen, occurs outside of your period, or is accompanied by very heavy bleeding, see your gynecologist. There could be an underlying cause such as endometriosis or adenomyosis. If you have questions about what a normal period is, you can read more in this article.
Taken occasionally and at recommended doses, ibuprofen is safe for most people. Additionally, by blocking the production of prostaglandins, it acts on the cause of the pain, not just the symptom. If you have gastric issues, ulcers, or take other medications, consult your doctor before using it regularly.
Foods with anti-inflammatory properties are the most useful: fatty fish, nuts, ginger, turmeric, and leafy greens like spinach or kale. Reducing sugar, alcohol, and caffeine in the days leading up to your period can also make a difference.
It doesn't act directly on the pain, but many of our users report less discomfort than with tampons. This may be because our menstrual cup does not absorb the natural moisture of the vaginal mucosa nor create internal pressure, unlike tampons. If you want to explore other options, we also have a menstrual disc.



