
Complete guide to pubic hair removal without irritation
5 de March de 2026
Women’s Wellness Books: Reads to Understand Your Body and Nurture Your Emotions
6 de March de 2026
Cystitis is one of those discomforts that many women know all too well. That burning sensation when urinating, the constant urge to go to the bathroom with little result, the pressure in the lower abdomen… These are signals that the body sends, and it’s important to know how to interpret them.
In this article, we review the most common symptoms of cystitis, what causes it, how it relates to intimate hygiene and menstruation, and when it’s important to seek medical evaluation. It’s not about panicking, but rather understanding what’s happening and acting with information.
What is cystitis and why is it so common in women
Cystitis is an inflammation of the bladder, usually caused by a bacterial infection. In most cases, the responsible bacteria is Escherichia coli (E. coli), which naturally resides in the intestine but can migrate to the urinary tract.
Women are significantly more prone to it than men. The main reason is anatomical: the female urethra is shorter and located closer to the anus, making it easier for bacteria to reach the bladder. In fact, it is estimated that between 50% and 60% of women will experience at least one episode of cystitis in their lifetime.
It is not a serious illness in most cases, but it can be bothersome, recurrent for many women, and may complicate if not addressed in time.
Symptoms of cystitis: how to recognize it
The symptoms of cystitis usually appear suddenly and are quite recognizable. Although the intensity varies from person to person, these are the most common signs:
- Burning or stinging sensation when urinating, especially at the beginning or end of urination.
- Frequent urge to go to the bathroom, even when the bladder is practically empty.
- Feeling of not having completely emptied the bladder after urination.
- Cloudy urine, with a stronger odor than usual or, in some cases, with the presence of blood.
- Pressure or pain in the lower abdomen, at the level of the pubis.
- General discomfort, with irritability or fatigue during more intense episodes.
In some cases, especially if the infection progresses without treatment, fever, lower back pain, or nausea may occur. These symptoms may indicate that the infection has reached the kidneys (pyelonephritis) and require urgent medical attention.
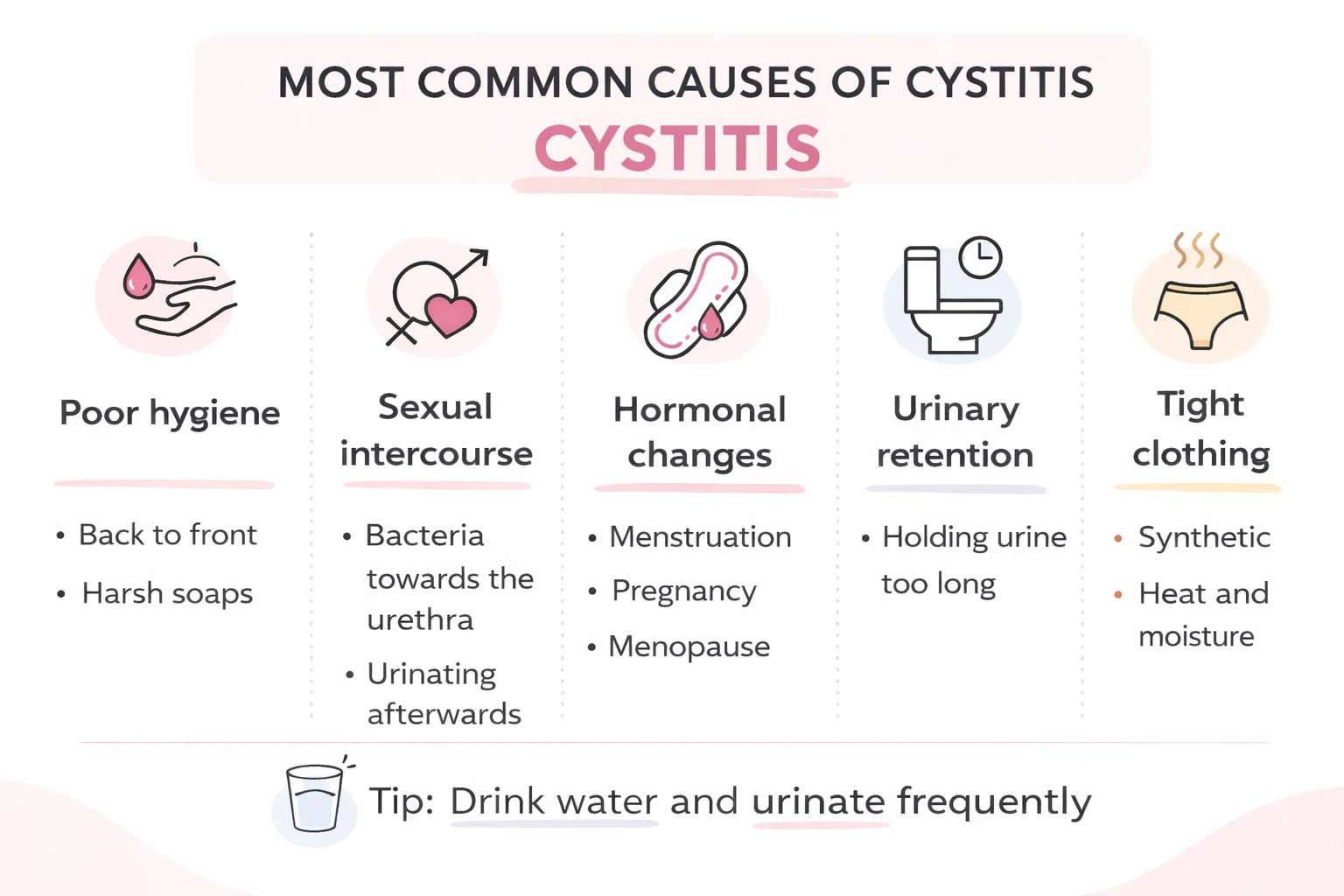
Most common causes of cystitis
Cystitis can occur for multiple reasons, although there is almost always a common denominator: the presence of bacteria in the urinary tract. Below, we review the factors that most frequently contribute to its occurrence.
Inadequate intimate hygiene
Improper cleaning of the genital area is one of the most direct causes. Wiping from back to front after using the bathroom makes it easier for intestinal bacteria to reach the urethra. The correct direction is always from front to back.
The use of harsh soaps, vaginal douches, or perfumed products that alter the natural pH of the intimate area also plays a role. When the vaginal flora loses its balance, pathogenic bacteria find less resistance to proliferate.
Sexual intercourse
Sexual intercourse is another frequent factor, to the point that there is a colloquial term "honeymoon cystitis." During sexual activity, bacteria present in the genital area can move toward the urethra. That’s why it is recommended to urinate after sexual intercourse as a preventive measure.
Hormonal changes and menstruation
The hormonal changes that occur during the menstrual cycle, pregnancy, or menopause can alter the conditions of the vaginal and urethral mucosa, reducing the natural defenses of the area. During menstruation, moreover, prolonged moisture in the intimate area and contact with disposable menstrual hygiene products can promote the occurrence of infections.
The use of tampons or pads for many hours creates a warm and moist environment that facilitates bacterial proliferation. Therefore, it is advisable to change them frequently and consider alternatives that do not alter the vaginal pH, such as the menstrual cup or the menstrual disc, which collect the flow without absorbing it and are made of medical-grade silicone.
Urine retention
Holding in the urge to urinate for prolonged periods allows bacteria to remain in the bladder longer, increasing the risk of infection. Drinking enough water and maintaining a regular urinary frequency is one of the simplest preventive measures.
Wearing tight or synthetic clothing
Underwear made of synthetic materials and very tight clothing limit the ventilation of the genital area. This combination of heat and moisture creates favorable conditions for bacterial development. Cotton underwear and loose-fitting garments help keep the area more ventilated.
Cystitis and Menstruation: A Relationship Worth Understanding
Menstruation and cystitis coincide more often than one might think. During the period, hormone levels drop, and the intimate area becomes more vulnerable. The skin becomes sensitive, the mucosa can irritate more easily, and prolonged moisture increases the risk of urinary infections.
Disposable menstrual hygiene products, especially those containing synthetic materials, fragrances, or bleaches, can worsen this situation. Skin irritation during menstruation is a more common issue than is often discussed, and it is directly related to the type of product used.
Similarly, the odor during menstruation is not due to the menstrual flow itself but to the reaction of blood with air and absorbent materials. When using collection products like the menstrual cup or disc, which do not absorb or come into contact with air in the same way, both irritation and odor are significantly reduced.
When to Consult a Professional
Mild cystitis can resolve in a few days, especially if fluid intake is increased and good hygiene is maintained. However, there are situations where it is important to seek medical evaluation:
- Symptoms do not improve within two to three days.
- Fever, lower back pain, or chills appear.
- Urine consistently shows blood.
- Episodes recur frequently (more than two or three times a year).
- You are pregnant, as urinary infections during pregnancy can lead to complications.
The diagnosis is usually made through a urine test that confirms the presence of bacteria. From there, the healthcare professional will determine the most appropriate treatment, which typically includes short-term antibiotics.
Prevention: Small Habits That Make a Difference
Preventing cystitis does not require major changes but rather attention to daily habits. Maintaining adequate hydration, not holding urine longer than necessary, always wiping from front to back, and using intimate hygiene products with an appropriate pH are simple and effective measures.
During menstruation, choosing products that respect vaginal flora is especially relevant. The menstrual cup and the menstrual disc, made from medical-grade silicone, do not alter vaginal pH or create the moist environment that disposable products promote. This is an aspect that is not always considered but can influence the frequency of cystitis episodes.
If you want to learn more about how menstrual care can be part of your intimate health routine, at PapayaCup you will find information and products designed with that philosophy.
FAQ: Symptoms of Cystitis
No. It occurs when bacteria from the body access the urinary tract. It is not transmitted through contact.
Yes. There is interstitial cystitis, which causes similar symptoms without the presence of bacteria. It is less common and requires a specific diagnosis.
They contain proanthocyanidins, which can hinder the adhesion of bacteria to the bladder. They are a preventive supplement but do not replace medical treatment.
No. The menstrual cup is placed in the vaginal canal, independent of the urinary tract. Being made of medical silicone, it does not alter pH or promote bacterial growth.
Yes. It is made from surgical-grade silicone, hypoallergenic, and biocompatible. Unlike tampons, it does not absorb or dry out the intimate area, helping to maintain natural protective conditions.



